May 27, 2021
Why COVID cases in world's most immunized nation are rising despite vaccine push
, Bloomberg News

For epidemiologists, the past year and a half has been a voyage of discovery. Recently their journey aboard SARS-CoV-2 took an unexpected turn toward Seychelles, a palm-fringed archipelago in the Indian Ocean with fewer than 100,000 inhabitants. A country that few could pinpoint on a map suddenly became internet-famous as the most vaccinated nation on Earth, with 64 per cent of the population having received the requisite two shots. Yet to the surprise of virologists—and the dismay of the government, which had been counting on the immunization drive to reopen the tourism-dependent economy—the infection count has been ticking up. As of May 13 a third of active cases—about 900 in all—were among residents who’d been fully vaccinated.
Vaccine skeptics pronounced themselves vindicated, while international health experts have been scrambling to answer a host of questions without the benefit of robust data. Did one or both of the vaccines used in Seychelles fail? Has herd immunity not been reached? Is the nation grappling with a more infectious variant capable of evading the defenses that certain types of vaccines provide?
“So what’s going on?” asked Raina MacIntyre, professor of global biosecurity at the Sydney campus of the University of New South Wales, during an online presentation on May 18. “It’s probably that the herd immunity threshold hasn’t been reached, plus or minus, if it’s the South African variant in there.”
The answers to the questions MacIntyre and other experts are posing may influence the future course of the pandemic. For starters, the tiny nation has become a test case for two of the world’s most widely used vaccines. In the Seychelles, 57 per cent of the vaccinated population received Sinopharm’s shot, and 43 per cent got the Covishield vaccine developed by AstraZeneca Plc. Sinopharm’s inoculation has been donated or sold to countries around the globe, including Indonesia, Venezuela, and Zimbabwe; Covishield makes up the bulk of shots distributed to poor nations in Africa and elsewhere through the Covax initiative, which seeks to make vaccine distribution more equitable.
What’s happening in Seychelles is very different from the experience of Israel, the second-most vaccinated nation, where COVID-19 infections have plummeted. The contrast could yield crucial insights into the efficacy of the different types of immunizations. In Israel the dominant vaccine was the messenger ribonucleic acid shot made by Pfizer Inc. and BioNTech SE.
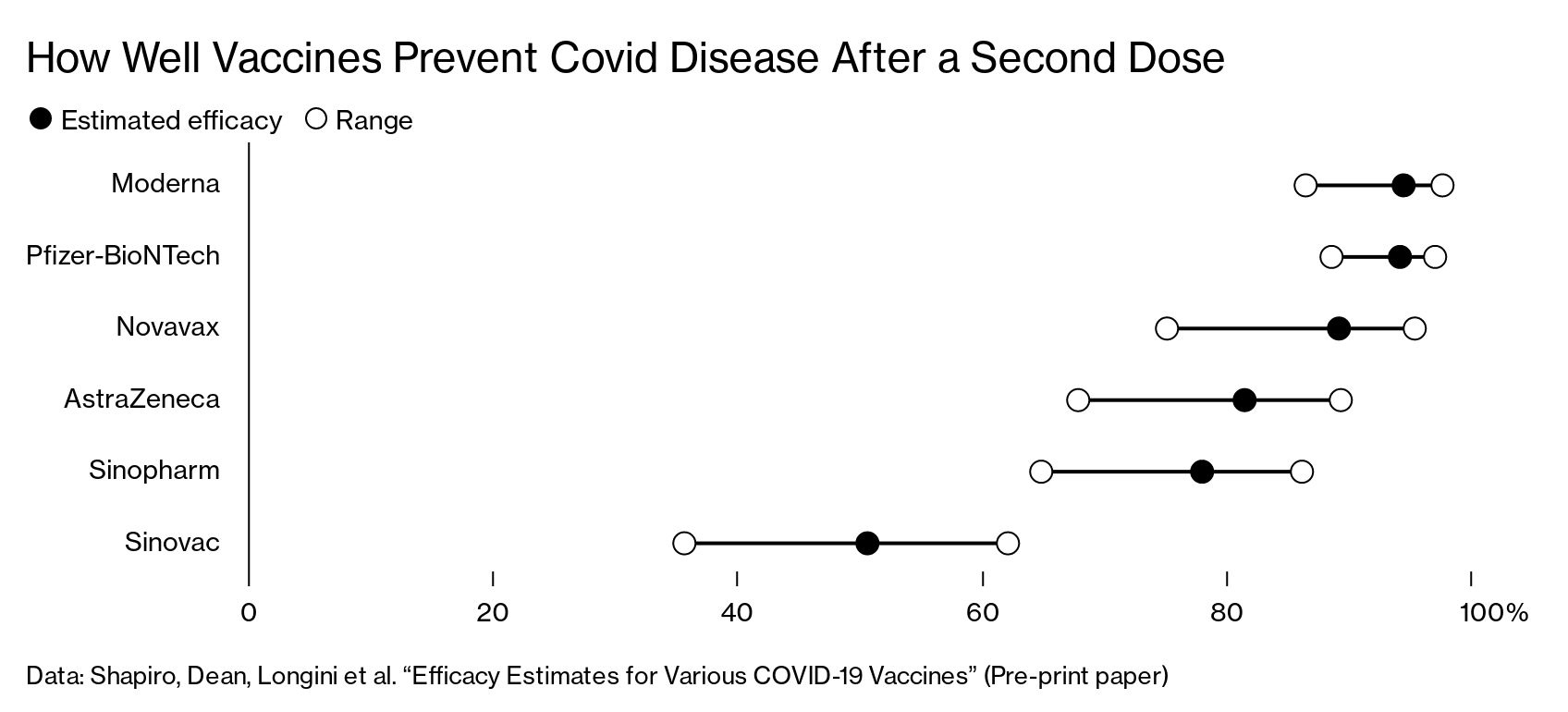
The pandemic has seen mRNA vaccines— Moderna Inc. makes another—being used in scale for the first time. Data from clinical trials so far suggest they are better at stopping Covid, tackling variants, and preventing the virus from spreading in the community. Sinopharm’s and AstraZeneca’s vaccines rely on more traditional methods, and their shots have been shown to have lower efficacy in studies.
What’s also apparent, so far, is that though there’s been a surge in cases in Seychelles, very few people are getting seriously ill. “We have only a few people needing intensive care. Two out of 40” in hospitals, said Seychelles President Wavel Ramkalawan in a May 10 interview. “The vaccine will protect people from getting serious symptoms.”
Still, more answers are needed. The government hasn’t disclosed what vaccine was administered in the breakthrough cases that make up a third of the total count. No agency has done any genomic sequencing to determine which variant is dominant on the islands, though the one first identified in South Africa, B.1.351, was detected in Seychelles in February.
On May 13, Jude Gedeon, the country’s public-health commissioner, said samples were to be sent to the Kenya Medical Research Institute for testing. The World Health Organization is also taking action. “We are very concerned, and we are sending a multidisciplinary team there to help the Seychelles government address the situation,” says Richard Mihigo, program area manager for immunization and vaccine development at the WHO’s regional office for Africa in Brazzaville, Republic of Congo. “We are also in discussion with the government to conduct a vaccine effectiveness study.”
The situation in Seychelles also offers a fresh reminder that our understanding of herd immunity—the theoretical threshold at which the virus can’t find enough hosts to keep spreading—continues to evolve. Scientists once estimated that 55 to 82 per cent of the population would need to have immunity against SARS-CoV-2, either from recovering from an infection or through vaccination. But 17 months into the pandemic, there’s recognition that the threshold may vary depending on the susceptibility of a population to the circulating strains, adherence to physical distancing, mask-wearing, and other practices known to reduce transmission, as well as the season—epidemics typically worsen as either colder or hotter weather encourages people to congregate indoors.
“It’s probably not likely that we are going to drive to zero the transmission of this virus or have it disappear,” says Jennifer Nuzzo, an epidemiologist and senior scholar at the Johns Hopkins Center for Health Security in Baltimore. Still, she see vaccines “doing the thing that we care most about, which is preventing serious illness.”
Lessons from Seychelles could be valuable to other countries in assembling their own vaccine arsenals, through purchases or donations—or a combination of the two, as the tropical nation did. “It’s about quality vaccines that are shown to be effective against your variant,” says Glenda Gray, president of the South African Medical Research Council and co-lead of a Johnson & Johnson Covid vaccine trial in the country.
Finance Minister Naadir Hassan, who had to steer Seychelles’s economy through a 13 per cent contraction in 2020, says the government cannot afford to stand still while it awaits answers to these COVID riddles. The country is “an open, vulnerable economy,” he said in a May 13 interview. “The country needs to be safe, and the country needs to be open.”
